Shingles (Herpes Zoster)
Fast Facts I For Your Patients I Shingles I Continuing Education
Fast Facts
- Painful rash, develops along a dermatome.
- Blisters typically scab over in 7 to 10 days, and clear up within 2 to 4 weeks.
- Post-herpetic neuralgia (PHN) is the most common complication.
- Risk increases with age and chickenpox infection.
- CDC recommends a single dose of herpes zoster vaccine for people 60 years and older.
For Your Patients
Shingles Fact Sheet: English
Vaccine Information Statement: English | Spanish
Infographic: here
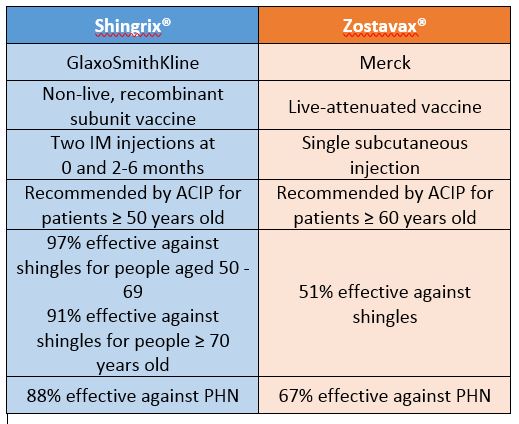
From the CDC: There are currently ordering limits and intermittent shipping delays for GlaxoSmithKline’s Shingrix vaccine (Recombinant Zoster vaccine) due to high demand. Until demand can be met, it is particularly important that vaccine providers educate patients about the importance of completing the series. In addition, CDC reminds health care professionals of proven strategies to help patients receive all their needed vaccinations on time, including Shingrix:
- Implement a vaccine reminder and recall system using phone, e-mail, or text messages to contact patients when you have Shingrix supply. Give first consideration to patients due for their second dose of Shingrix (https://www.thecommunityguide.org/findings/vaccination-programs-client-reminder-and-recall-systems).
- If you are out of Shingrix and a patient needs a second dose, refer the patient to another provider in the community (e.g., a pharmacy) that has Shingrix so the patient can complete the series. The immunization program at your state or local health department or vaccine finder can help identify other immunization providers (https://vaccinefinder.org).
- Be sure to enter your patients’ current vaccination information into your state’s immunization information system (IIS). This will ensure that every provider can access your patients’ immunization record, and it may help facilitate patient reminders to complete the Shingrix series.
- As supply becomes less constrained, be sure to notify eligible patients so they can come in to get their first dose of Shingrix.
Timely series completion is key to the success of any vaccination program and critical to ensuring patients receive the full benefit of their vaccinations.
Shingles (Varicella Zoster Virus)
From the CDC’s Pink Book.
VZV is a DNA virus and is a member of the herpesvirus group. Like other herpesviruses, VZV has the capacity to persist in the body after the primary (first) infection as a latent infection. VZV persists in sensory nerve ganglia. Primary infection with VZV results in chickenpox. Herpes zoster (shingles) is the result of reactivation of latent VZV infection. The virus is believed to have a short survival time in the environment.
VZV enters through the respiratory tract and conjunctiva. The virus is believed to replicate at the site of entry in the nasopharynx and in regional lymph nodes. A primary viremia occurs 4 to 6 days after infection and disseminates the virus to other organs, such as the liver, spleen, and sensory ganglia. Further replication occurs in the viscera, followed by a secondary viremia, with viral infection of the skin. Virus can be cultured from mononuclear cells of an infected person from 5 days before to 1 or 2 days after the appearance of the rash.
Herpes zoster, or shingles, occurs when latent VZV reactivates and causes recurrent disease. The immunologic mechanism that controls latency of VZV is not well understood. However, factors associated with recurrent disease include aging, immunosuppression, intrauterine exposure to VZV, and having had varicella at a young age (younger than 18 months). In immunocompromised persons, zoster may disseminate, causing generalized skin lesions and central nervous system, pulmonary, and hepatic involvement.
The vesicular eruption of zoster generally occurs unilaterally in the distribution of a sensory nerve. Most often, this involves the trunk or the fifth cranial nerve. Two to four days prior to the eruption, there may be pain and paresthesia in the involved area. There are few systemic symptoms.
Postherpetic neuralgia (PHN), or pain in the area of the ocurrence that persists after the lesions have resolved, is a distressing complication of zoster. There is currently no adequate therapy available. PHN may last a year or longer after the episode of zoster. Ocular nerve and other organ involvement with zoster can occur, often with severe sequelae.
top
Continuing Education
Varicella & Shingles Presentation, CDC: English (8/02/2013)
Shingrix Information: MMWR 67 (3): English (1/26/2018)
Shingrix Information: English
top